Last Updated on March 30, 2026 by Jordyn Koveleski Gorman
If your infant or toddler has recently been diagnosed with a lip and/or tongue tie, there’s a few things you need to know about treatment before getting started.
First things first: the internet is not a diagnostician, and pediatricians are amazing and so important, but are also not specialists in this area. If the diagnosis came from either of those places, it’s time for a specialist follow up!
Not sure if your little one has a lip or tongue tie? You can review signs of lip and tongue ties on our blog. It’s important to note that ties cannot be diagnosed based on just the appearance inside the mouth. Function impairment is a necessary part of establishing a diagnosis!
Our team of child development specialists, including speech-language pathologists, feeding specialists, and a breastfeeding specialist, have put their expertise together in this blog to help parents understand the course of treatment for lip and tongue ties.
What are lip and tongue ties?
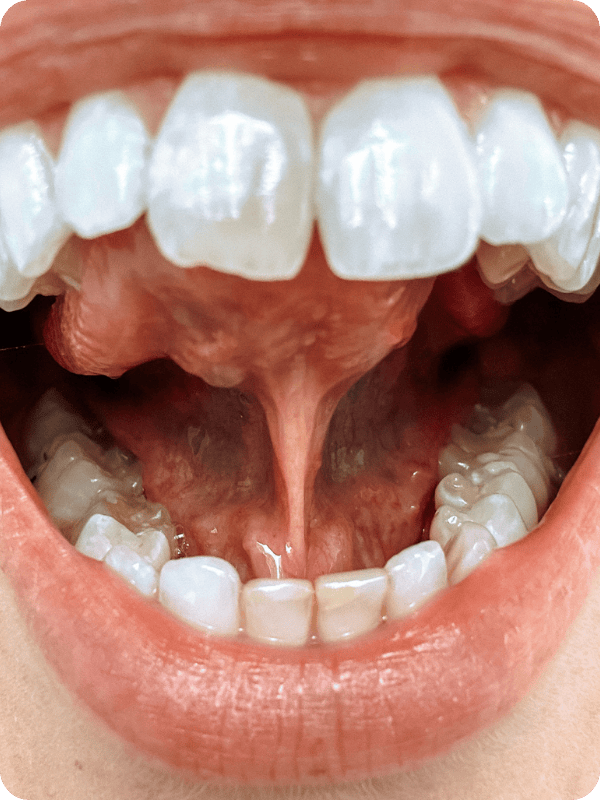
Tongue and lip ties are pieces of tissue, called frenula, made from collagen and/or muscular fibers, that restrict proper oral function. Without good movement and stretching abilities, functional impacts while feeding will be observed.
Frenula impact how the tongue, lips, and cheeks move for sucking, swallowing, eating solids, and breathing. If the tissue has ample movement and good stretch, there should be no functional impacts.
Tongue, lip, and cheek ties are still relatively new to clinical research. What is being seen in clinical practice is driving current research studies. While anecdotal evidence is not a very strong form of evidence, it’s important to remember that clinical practice is where research begins.
What we know so far from the research is that there isn’t a lot of strong evidence supporting that oral ties should be released.
Many providers in the past (and even now) have jumped right to releasing ties without recommending therapy before and after the release. As a result, sometimes outcomes aren’t always as good as they could be. Ensuring that parents understand the entire process and are aware that releasing a tongue/lip tie is not a one-size-fits-all procedure is important.
Before diving into the step-by-step treatment process below, let’s discuss some frequently asked questions about lip and tongue ties.
Do tongue, lip, and cheek ties stretch on their own over time?
No. The frenulum of the tongue, lips, or cheeks are made of connective tissue, collagen, and sometimes combined with muscular fibers. They are unable to stretch on their own. The tissue around the frenula can soften and increase in mobility, but the frenulum itself will not stretch on its own. (1)
Do the issues associated with tongue/lip/cheek ties correct themselves over time?
While the symptoms associated with ties can change, we often see them compound over time.
It’s important to know that the body wants to do what is easiest. Compensations like mouth breathing, sticking to soft or meltable foods, and sleep disordered breathing form in the absence of proper structure. Knowing the root cause of your child’s oral motor issues is part of making an informed decision about how to move forward! (2)
Are tongue/lip/cheek ties new and overdiagnosed?
Restricted frenula have been recognized and treated since the Middle Ages to help with feeding and speech. Prevalence of tongue ties is estimated to be around 8%, but this may not fully take into account posterior lingual restrictions, as those can be harder to spot. (3)
Controversies have been present regarding who should treat and release ties, along with the effectiveness of frenectomies. Despite availability of several assessment measures, there still is a lack of consistent, standardized assessment among medical professionals.
The best way to assess the root cause of feeding difficulties is involving multiple trained professionals reviewing medical history and observing the infant at rest and while feeding. Unfortunately, that means that evaluation and treatment are not quick. But, we want things done right, not fast, so in a way this is a good thing.
Considering how much is involved in evaluation of ties, it seems plausible that inaccurate, inconsistent diagnostics may lead to both over- and under-diagnosing.
We also know that a frenectomy, or a tie release, alone is often not enough to create long-term changes in functional movement. Clinical success often involves ensuring mom and baby get support, along with a combination of pre- and post-operative therapy that focuses on the whole body.
Do tongue ties only affect breastfeeding? Not bottlefeeding?
Most research supports that addressing tongue ties can reduce maternal pain and improve breastfeeding efficiency. Additionally, clinicians often see that tongue ties can impact the quality and control of sucking, which can impact bottle feeding.
Bottle feeding can also “mask” a tongue tie’s true impact, especially when using a bottle that relies on a shallow latch and compression. But, there is research to show that bottle feeding skills improved post frenectomy. (4) So, this answer is not so black-and-white.
If your baby has excessive gassiness, clicking/loss of suction, leaking of milk on the lips, milk residue on their tongue after feeding, chronic spit up, or uncoordinated bottle feeds, it’s important to get a full structural and function assessment by an IBCLC and/or therapist (SLP, OT).
Treatment for lip and tongue ties
If it is determined that your baby or child has signs and symptoms of tongue, lip, and/or cheek ties, your evaluating therapist should be able to support you through the process of pre-operative therapy and post-operative therapy.
Lip and tongue tie therapy
An evaluating therapist may notice and observe tension patterns impacting jaw, head, and body movements, which can warrant a referral to a bodywork professional. That may be a physical therapist, occupational therapist, chiropractor, or professional trained in craniosacral therapy.
Bodywork may relieve all of the signs and symptoms of a tongue tie. Or, it may resolve some of them and lead to further investigation on if a tongue tie release is warranted.
Frenectomy for lip and tongue ties
A bodywork professional can refer you to a release provider, and they also will help determine the right timing of frenectomy(ies) for your child and family. Frenectomies are a 6+ week process in most cases.
Getting a frenectomy (tongue/lip/cheek tie release) without therapy may not give the results you’re looking for. Before and after the extra tissue is released, the tongue must learn how to move differently. This is where therapy matters.
Because the process of identifying a tongue tie can be confusing, we wrote out the steps to follow to ensure that your child is receiving the best care. In the case of lip and tongue ties, this also means ensuring that you’re not receiving a release that is unwarranted or that is too soon!
The process of a tongue tie release
We’ve found the following “steps” work best to maximize results when a tongue/lip/cheek tie is identified:
- Receive a functional oral-motor structural and skill assessment by an SLP, IBCLC, and/or OT.
- Receive bodywork to assess and optimize tension patterns and movement. This should be with a physical therapist, occupational therapist, chiropractor, or a professional trained in craniosacral therapy.
- Receive a consultation with a recommended frenectomy provider for infants and/or children (usually dentist or ear-nose-throat doctor/otolaryngologist) if signs and symptoms persist after receiving oral-motor and body work therapy.
- Initiate or continue oral-motor (and whole-body) therapeutic exercises and have open discussions about progress with your therapist.
- Determine whether any frenectomies are warranted at this time, and if so, schedule them.
- Complete frenectomies and begin active wound care stretches as recommended by your release provider.
- Continue oral-motor and whole-body treatment as recommended through and after the healing process, for at least 4 weeks.
All in all, we see that the older the baby is, the longer they may need support. This is simply due to the fact that they’ve been compensating and using less-than-optimal motor plans for a longer period of time.
This is part of why, at Eat Play Say, we recommend asking questions early and seeking support as soon as your parent gut kicks in.
If you don’t feel like your questions are being validated and answered, a second opinion from another provider doesn’t hurt. This isn’t a decision to be made quickly—it’s one to make after receiving education.
More infant and toddler support
Whether your little one is a newborn or nearing preschool, we’ve got resources to help. Parenting is hard, and you deserve support!
You can find information about breast and bottlefeeding, starting solids, and development on our blog. And if you’re struggling to find ways to play with your little one, we’ve got ideas for days in our play category!
For more in-depth support and resources you can carry in your pocket, check out our Handbooks! Written by developmental specialists and yours for life, our Handbooks leave no stone unturned in your journey of parenthood.
Sources
- Mills N, Pransky SM, Geddes DT, Mirjalili SA. What is a tongue tie? Defining the anatomy of the in-situ lingual frenulum. Clin Anat. 2019 Sep;32(6):749-761. doi: 10.1002/ca.23343. Epub 2019 Feb 19. PMID: 30701608; PMCID: PMC6850428.
- Ghaheri BA. 2016. Breastfeeding Compensations for Tongue Lip Tie Are Problematic. https://www.drghaheri.com/blog/2016/6/23/breastfeeding-compensations-for-tonguelip-tie-are-problematic
- Hill, R.R., Lee, C.S. & Pados, B.F. The prevalence of ankyloglossia in children aged <1 year: a systematic review and meta-analysis. Pediatr Res 90, 259–266 (2021). https://doi.org/10.1038/s41390-020-01239-y
- Ghaheri BA, Lincoln D, Mai TNT, Mace JC. Objective Improvement After Frenotomy for Posterior Tongue-Tie: A Prospective Randomized Trial. Otolaryngology–Head and Neck Surgery. 2022;166(5):976-984. doi:10.1177/01945998211039784